A 12-week, Multicenter, Randomized, Double-blind, Placebo-controlled Clinical Trial Evaluating the Efficacy and Safety of DKB-131 in Knee Arthritis
Abstract
In this study, the efficacy and safety of DKB-131 (extract of Siraitiagrosvenorii) in adults of both genders presenting mild symptoms of knee arthritis were evaluated in comparison to a placebo. This clinical trial was randomized, double-blind, multicenter, and lasted for 12 weeks. A total of 120 participants with Visual Analogue Scale (VAS) scores of 30 mm or higher in the knee area and Kellgren & Lawrence Grade I or II knee arthritis on X-ray were enrolled, with 60 subjects randomized to receive DKB-131 and 60 subjects receiving placebo. Following 12 weeks of consumption, the change in K-WOMAC total score assessed in the per protocol (PP) set revealed a reduction of 21.86±15.98 points in participants who received DKB-131 (p<0.0001), whereas those in the placebo group exhibited a reduction of 14.92±16.66 points (p<0.0001). This demonstrated a statistically significant difference between the test groups (p=0.0389). Additionally, significant differences were observed between the DKB-131 and placebo groups in the changes in K-WOMAC pain (p=0.0157) and physical function (p=0.0447). For the secondary efficacy endpoint, the change in Visual Analogue Scale (VAS) scores, analyzed in the PP set after 12 weeks of consumption, the test group showed a reduction of 17.82±13.80 mm (p<0.0001), while the control group exhibited a reduction of 11.81±13.99 mm (p<0.0001), indicating a statistically significant difference between the test groups (p=0.0359). Safety evaluations including hematological tests, biochemical tests, and urinalysis revealed no clinically significant differences between the consumption groups. Additionally, vital signs (pulse, blood pressure) and anthropometric measurements (body weight) did not exhibit clinically significant differences between the consumption groups, confirming the safety of DKB-131. We propose that the consumption of DKB-131 is safe for humans and may contribute to joint health. Trial registration (CRIS.NIH.go.Kr): KCT0008527
Author Contributions
Academic Editor: Derek Ball, School of Life Sciences Heriot-Watt University Edinburgh, UK.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2024 Hee Jeong Eom, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Joints are areas where two or more bones come together, and the ends of the bones forming a joint are covered with cartilage, which allows smooth movement and prevents them from rubbing against each other. When cartilage is damaged, abnormalities may occur in the bone beneath it. Inflammation typically occurs in the process of cartilage degradation. With aging, cartilage may deteriorate, leading to deformation of the joint and localized degenerative changes. Degenerative joint disease, also known as osteoarthritis, arises from degenerative changes in joint cartilage, with pain being the primary symptom.
The World Health Organization (WHO) defines osteoarthritis as a condition that both causes disability in daily life due to pain and functional impairment and leads to physical and psychological problems such as depression, helplessness, and social isolation. In the domestic context, osteoarthritis is reported as a significant disease causing economic loss in the elderly population.1
Osteoarthritis, a prevalent national disease affecting approximately 20% of the global population, manifests as degenerative changes in the joints. While osteoarthritis can affect all joints, the knee joint is particularly susceptible, being the most commonly affected site. Involvement of the knee joint significantly limits everyday activities such as walking, sitting, and climbing stairs, leading to functional impairments.2
Treatment options for osteoarthritis of the knee, also known as degenerative knee arthritis, include surgical interventions, lifestyle modifications, exercise, complementary and alternative therapies, and pharmacotherapy. The Korean Orthopedic Association recommends management strategies such as weight loss and physical activity for the management of degenerative knee arthritis.3 Medications commonly used for the treatment of osteoarthritis include acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs). However, acetaminophen carries a potential risk of liver damage, while NSAIDs pose risks of gastrointestinal complications such as ulcers and perforations.4
In light of the concerns surrounding side effects and the long-term burden of conventional medications for osteoarthritis, there has been a significant increase in demand for health functional foods targeting joint health in recent years. Reflecting this trend, 13% of the total production value of individually recognized health functional foods in South Korea in 2010 comprised products aimed at joint and bone health, indicating a high proportion in this category.5
S. grosvenorii, commonly known as monk fruit or Luo Han Guo in Chinese, is a deciduous tree native to China. It is often referred to as the "fruit of god" due to its various health benefits. Luo Han Guo contains essential vitamins such as A, C, and E, as well as various minerals vital for maintaining health. One of its distinctive features is its unique sweet taste, derived from triterpene glycosides rather than sugars. These glycosides are not absorbed in the intestines and are excreted directly, resulting in negligible calorie content. Moreover, these compounds have been reported to promote the activity of beneficial bacteria in the gut, contributing to gastrointestinal health.6, 7 Furthermore, Luo Han Guo contains all eight essential amino acids, with glutamate being the predominant constituent amino acid, and it also contains a small amount of γ-aminobutyric acid (GABA). In addition to these, Luo Han Guo is rich in phytochemicals such as flavonoid glycosides, campesterol, quercetin, polyphenolic compounds, and β-sitosterol. These compounds contribute to its health-promoting properties, making Luo Han Guo a valuable food ingredient with potential health benefits. 8, 9, 10
Materials and Methods
DKB-131 Preparation
The manufacturing process of DKB-131 (Dongkook Pharmaceutical Co., Ltd., Suwon, Korea, Lot number: LHGE-210417) functional ingredient is as follows. The dried residue of S. grosvenorii was extracted twice using 70% ethanol, followed by filtration and vacuum concentration. The resulting extract was then mixed with food-grade maltodextrin and dried to obtain a powdered sample. Subsequently, the sample was uniformly ground to produce S. grosvenorii extract powder, the functional ingredient. The test food consisted of DKB-131 functional ingredient (375 mg) encapsulated in a white hard capsule (500 mg), containing crystalline cellulose, calcium carboxymethyl cellulose, silicon dioxide, and magnesium stearate. The control food (500 mg) contained maltodextrin, crystalline cellulose, calcium carboxymethyl cellulose, silicon dioxide, and magnesium stearate.11
Both the test and control foods were manufactured by RP Bio Inc. (Gyeonggi-do, South Korea) in a facility certified with Good Manufacturing Practice (GMP) standards.
Study Design
This study was conducted as a randomized, double-blind, placebo-controlled parallel trial with a 3-month follow-up period. The protocol was registered on August 3, 2022, with NeoNutra Co., Ltd. located in Jongno, Seoul, Republic of Korea (Protocol number: DKB-131-HS, Version 2.1), sponsored by Dongkook Pharmaceutical Co., Ltd. Participants were recruited from Inje University Seoul Paik Hospital, Seoul Metropolitan Boramae Hospital, and Hallym University Sacred Heart Hospital. The study was conducted in accordance with the Helsinki Declaration and International Conference on Harmonization of Good Clinical Practice (ICH GCP) guidelines. The protocol received independent review and approval from the Institutional Review Board (IRB) of each participating institution (Project Identification Code: DKB-131-HS, Approval Number: PAIK 2021-10-002; CRIS.NIH.go.Kr ID: KCT0008527).
Participants who voluntarily signed the informed consent form for participation in this clinical trial underwent various assessments and screenings to determine their eligibility. These assessments included demographic surveys, lifestyle questionnaires, medical history and medication usage surveys, physical examinations, vital sign measurements (blood pressure, heart rate), anthropometric measurements, X-ray imaging, clinical pathology tests, and pregnancy tests (for women of childbearing age). Additionally, Visual Analogue Scale (VAS) evaluations were conducted. Eligible participants were then randomly assigned to either the test group or the control group and consumed the test food or control food for a total of 12 weeks.
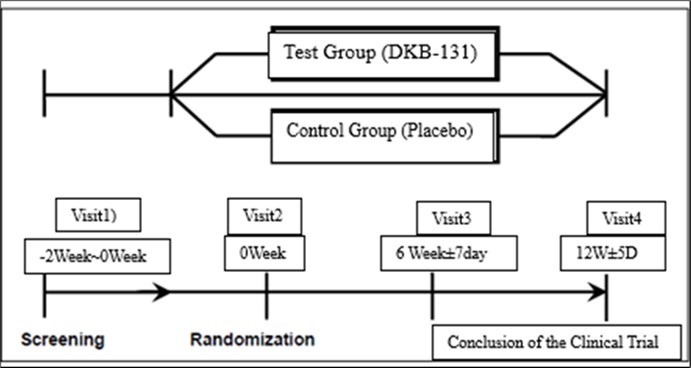
During the course of the trial, spanning from Visit 2 to Visit 12, participants were instructed to maintain their usual dietary habits, physical activity levels, and dietary intake, while avoiding regular consumption of Luo Han Guo-related foods. Dietary assessment forms were distributed to participants during Visits 2 and 3 to record their usual dietary intake throughout the trial period. During Visits 3 and 4, trial coordinators verified the dietary assessment forms completed by the participants. Participants visited the hospital a total of four times during the study period. Evaluations were scheduled at screening (-2 weeks to Week 0), baseline (Week 0), midpoint (Week 6 to Week 7), and final (Week 12) visits. The flowchart of the trial is depicted in Figure 1.
Ethics Approval and Consent of the Participants
The trial protocol (DKB-131-HS, Version 2.1, dated August 3, 2022) received approval from the Institutional Review Boards (IRBs) of Inje University Seoul Paik Hospital, Seoul Metropolitan Boramae Hospital, and Hallym University Sacred Heart Hospital. Before the start of the clinical trial, participants were provided with information about the nature, scope, and expected outcomes of the study, and written consent was obtained. All clinical trial participants' identities were kept confidential, and they were identified and recorded only by the assigned numbers during the trial. Participants were informed that all test data would be stored on computers and treated with strict confidentiality.
Participants
Inclusion Criteria
Participants who met all the following criteria were selected as subjects for the clinical trial.
Individuals aged 40 years or older but younger than 80 years, regardless of gender.
Individuals whose VAS (Visual Analogue Scale) scores, conducted during Visits 1 and 2, were 30 mm or higher (in the knee area).
Individuals whose Kellgren & Lawrence Grade on X-ray imaging of the knee joint corresponded to Grade I or Grade II.
Individuals who provided informed consent and completed the written Informed Consent Form before the start of the clinical trial.
Exclusion Criteria
Individuals who met any of the following criteria were excluded from participation as subjects in the clinical trial.
Individuals currently undergoing treatment for severe cardiovascular, immune, respiratory, hepatobiliary, renal and urological, neurological, musculoskeletal, infectious diseases, or malignant tumors.
Individuals with joint disorders due to specific factors other than degeneration, as determined by the investigator.
Patients with mental illnesses such as schizophrenia, depression, substance abuse, or alcohol-related disorders.
Individuals with gastrointestinal disorders that could interfere with the consumption of test foods for the clinical trial.
Individuals who had used intra-articular hyaluronate, glucocorticoids, or other medications within 3 months (90 days) prior to Visit 1.
Individuals who had used medications related to arthritis or health functional foods targeting joint health within 1 month (30 days) prior to Visit 1.
Individuals who received non-narcotic analgesics (such as acetaminophen, tramadol) and non-steroidal anti-inflammatory drugs orally or by injection within 2 weeks prior to Visit 1.
Individuals who started taking low-dose aspirin (100 mg) within 3 months (90 days) prior to Visit 1.
Those who received physical therapy or traditional Korean medicine treatment (acupuncture, moxibustion, cupping, etc.) for the treatment of osteoarthritis within 2 weeks prior to Visit 1.
Patients with uncontrolled hypertension (systolic blood pressure ≥ 160 mmHg or diastolic blood pressure ≥ 100 mmHg, measured after 10 minutes of rest)
Patients with uncontrolled diabetes (HbA1c ≥ 7.0%).
Individuals with AST (GOT) or ALT (GPT) levels exceeding three times the upper limit of normal at the participating institution.
Individuals with creatinine levels exceeding twice the upper limit of normal at the participating institution.
Individuals who participated in another interventional clinical trial (including clinical trials involving humans) within 1 month (30 days) prior to Visit 1 or planned to participate in another interventional clinical trial (including clinical trials involving humans) after the start of this clinical trial.
Women pregnant, lactating, or planning to become pregnant during the study period.
Individuals sensitive to the components of the test food for this clinical trial or with allergies.
Individuals deemed ineligible for other reasons by the investigator.
Withdrawal and Dropout
Cases where the clinical trial was discontinued for ongoing trial subjects include:
Violation of inclusion/exclusion criteria.
Use of concomitant prohibited medications, foods, or therapies.
Other significant violations considered to be in breach of the protocol.
Randomization and Blinding
The randomization table was generated using SAS® system's randomization program, which applied the permutation of random numbers (Random number A and B) to the sequential participant numbers from 1 to the total number of subjects. This was pre-designed and created using SAS® before the start of the clinical trial. Suitable subjects for this clinical trial were assigned consecutive participant numbers as follows, and each participant was instructed to consume the test food corresponding to their assigned serial number. To achieve balanced randomization between the test groups, participants were evenly distributed in a 1:1 ratio.
Throughout the study duration, neither the participants nor the research personnel had access to allocation information (regarding randomization). No unblinding occurred until the completion of the clinical trial.
Intervention
Participants were instructed to take 4 capsules daily for 12 weeks, consuming a total of 2 grams per day (1.5 grams of DKB-131 functional ingredient per day) after meals. The dosage administered in the human trial was determined based on previous efficacy tests conducted in animal models. In monosodium iodoacetate (MIA) induced animal models, pain suppression was observed with doses of 150 mg/kg bw/day and 200 mg/kg bw/day of the DKB-131(Luo Han Guo extract powder). From the 7th day of MIA-induced osteoarthritis in the animal model, the doses of DKB-131(Luo Han Guo extract powder) were calculated to be approximately 24.19 mg/kg and 32.26 mg/kg, respectively. Translated to a 60 kg adult, this equated to approximately 1.44 g to 1.92 g dosages. In the human trial, capsules containing 375 mg of DKB-131(Luo Han Guo extract powder) were administered once daily, four capsules per dose, to evaluate its effects. Table 1
Table 1. Clinical Trial Flowchart| Period | Screening | Active Treatment | |||
|---|---|---|---|---|---|
| Visit | 1 | 2 | 3 | 4 | |
| Week | -2 | 0 | 6 | 12 | |
| Window period(day) | ±7 | ±5 | |||
| Informed Consent | √ | ||||
| Demographic Survey | √ | ||||
| Lifestyle Assessment | √ | √ | |||
| Medical History and Medication History | √ | √ | |||
| Physical Examination | √ | √ | √ | ||
| Vital Signs (Blood Pressure, Pulse) | √ | √ | √ | ||
| Anthropometric Measurements (Height, Weight) | √ | √ | √ | ||
| Radiographic Imaging (X-ray) | √ | ||||
| Clinical Laboratory Tests | √ | √ | |||
| Pregnancy Reaction Test | √ | ||||
| Efficacy Evaluation | K-WOMAC | √ | √ | √ | |
| VAS | √ | √ | √ | √ | |
| SF-36 | √ | √ | √ | ||
| Self-assessment of Improvement in Trial Participants | √ | √ | |||
| Self-assessment of Improvement in Trial Subjects | √ | √ | |||
| ESR, CRP | √ | √ | |||
| Dietary Guidance and Dietary Survey | √ | √ | √ | ||
| Assessment of Eligibility of Trial Participants | √ | √ | |||
| Randomization | √ | ||||
| Prescription of Trial Intervention | √ | √ | |||
| Adverse Event Monitoring | √ | √ | |||
| Adherence Assessment | √ | √ | |||
| Evaluation of Changes in Concomitant Medications and Therapies | √ | √ | |||
| Self-assessment Surveys | √ | ||||
Prohibited Concomitant Drugs and Therapies
The following medications and therapies were restricted during the clinical trial to avoid interference with the safety, efficacy, and tolerability evaluation of the investigational drug:
1) Contraindicated Medications
Intra-articular hyaluronate, glucocorticoids, and other pharmaceuticals for joint administration
Non-opioid analgesics (such as acetaminophen, tramadol) and non-steroidal anti-inflammatory drugs (NSAIDs) used for arthritis
Low-dose aspirin (100 mg) (however, ongoing use initiated more than 3 months (90 days) prior to the start of the trial was allowed)
Nutraceuticals targeting joint health
Herbal remedies containing ingredients such as ginseng, astragalus, and licorice
2) Contraindicated therapies
Physical therapy or traditional Korean medicine therapies (such as acupuncture, moxibustion, and cupping) for the treatment of osteoarthritis
Outcome Evaluation
Primary Outcomes
The change in K-WOMAC total score and individual item scores evaluated at 6 and 12 weeks post-treatment compared to baseline was assessed. The degree of improvement was evaluated to determine if there was a statistically significant difference between the DKB-131 group and the Placebo group.
Secondary Outcomes
The change in VAS scores at 6 and 12 weeks post-treatment compared to baseline was assessed. The degree of improvement was evaluated to determine if there was a statistically significant difference between the DKB-131 group and the Placebo group.
Safety Outcomes
Safety evaluation variables included adverse events, vital signs (blood pressure, heart rate), anthropometric measurements (body weight), and clinical laboratory tests (hematological/serum chemistry tests, urine analysis).
Sample Size
The calculation of the sample size for this clinical trial was based on the significant effects observed in a previous study using the WOMAC assessment tool, as reported by Eytan M Debbi et al. Considering an anticipated dropout rate of 25% in the trial, it was determined that 60 subjects per group would be required for adequate efficacy evaluation. Therefore, a total of 120 subjects would be enrolled, with 60 participants allocated to each group.
Statistical Analysis
Statistical analysis was performed using SAS (Version 9.4, SAS Institute, Cary, NC, USA). Data related to efficacy, demographic and nutritional information, and safety were analyzed using a significance level of 0.05 for two-tailed tests. A p-value of <0.05 was considered statistically significant for all analyses.
For the primary efficacy outcome, the change in total score and individual item scores of K-WOMAC before and after intervention was compared using a paired t-test for domestic comparisons. The magnitude of change between the intervention and control groups at each time point was evaluated for statistical significance using either a two-sample t-test or Wilcoxon rank sum test, depending on the satisfaction of normality assumptions. For the secondary efficacy outcome, the within-group comparison of changes in VAS scores before and after intervention was analyzed using a paired t-test. The magnitude of change between the intervention and control groups at each time point was assessed for statistical significance using either a two-sample t-test or Wilcoxon rank sum test, depending on the satisfaction of normality assumptions.
If there were statistically significant differences between groups in demographic and lifestyle survey data, and if these differences were clinically significant, a Generalized Linear Model (GLM) with the baseline characteristic as a covariate (equivalent to ANCOVA) was conducted to adjust for these baseline characteristics.
Results
The clinical trial was conducted from March 23, 2022, to April 10, 2023, at Inje University Seoul Paik Hospital, Boramae Medical Center of Seoul Metropolitan Government, and Hallym University Sacred Heart Hospital. Screening evaluations were performed on a total of 135 participants to select suitable candidates for the trial. Among them, 15 participants were excluded during screening, resulting in a total of 120 participants (60 in the test group and 60 in the control group) who were randomly assigned. During the trial, there were withdrawals from the test group by 1 participant, withdrawals from the control group by 1 participant, and 1 participant in the control group had an adverse event, leading to a total of 3 participants dropping out prematurely. Therefore, the trial was completed with a total of 117 participants (58 in the test group and 59 in the control group). Figure 2
Figure 2.Participation Status and Analyzed Group of Participants in the Clinical Trial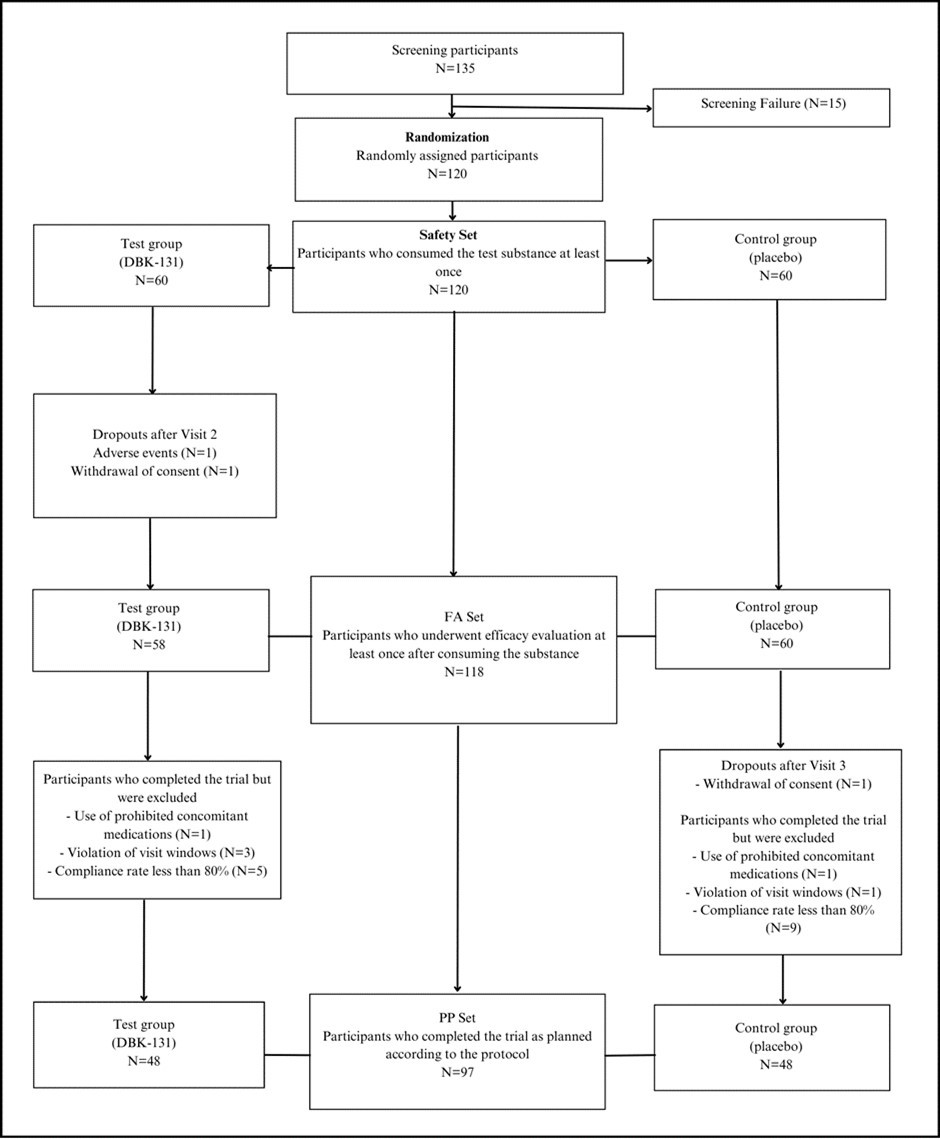
The per protocol (PP) set included a total of 97 participants (49 in the test group and 48 in the control group) who met the criteria for inclusion. This set comprised participants who completed the trial without any major protocol violations affecting the trial outcomes. Specifically, it included 1 participant (from the control group) who dropped out after Visit 3 without any significant protocol deviations, 14 participants (5 from the test group and 9 from the control group) with an average compliance rate of less than 80% as determined by the analysis group, 2 participants (1 from each group) who used prohibited concomitant medications, and 4 participants (3 from the test group and 1 from the control group) who violated the visit window by more than ±4 days at Visit 4.
The demographic characteristics and features of the participants before consumption in the trial were investigated. In terms of gender distribution, the test group comprised 11 males (22.4%) and 38 females (77.55%), while the control group included 5 males (10.42%) and 43 females (89.58%). However, no statistically significant difference was observed between the consumption groups. Regarding age, the test group had a mean age of 55.20±8.94 years, and the control group had a mean age of 54.63±9.73 years, with no statistically significant difference between the consumption groups. Additionally, there were no statistically significant differences observed between the groups in terms of fertility status, physical activity, smoking status, alcohol consumption, weight, and height, indicating comparability between the groups. Table 2
Table 2. Demographic Information and Pre-consumption Characteristics of Participants in the Clinical Trial (PP Set)| Test GroupN=49 | Control GroupN=48 | p-Value | ||
| Gender, n (%) | Male | 11 (22.45) | 5 (10.42) | (1)0.1104 (C) |
| Female | 38 (77.55) | 43 (89.58) | ||
| Age (years) | Mean±SD | 55.20±8.94 | 54.63±9.73 | (2)0.6833 (W) |
| Min, Max | 40.00, 70.00 | 40.00, 76.00 | ||
| Physical activity, n (%) | No | 8 (16.33) | 15 (31.25) | (1)0.176 (C) |
| 1-2 times/week | 10 (20.41) | 14 (29.17) | ||
| 3-4 times/week | 19 (38.78) | 13 (27.08) | ||
| 5-6 times/week | 8 (16.33) | 3 (6.25) | ||
| Every day | 4 (8.16) | 3 (6.25) | ||
| Smoking status, n (%) | No | 44 (89.80) | 46 (95.83) | (1)0.596 (F) |
| Quit smoking for more than 1 year | 4 (8.16) | 1 (2.08) | ||
| Quit smoking for less than 1 year | 0 (0.00) | 0 (0.00) | ||
| Currently smoking | 1 (2.04) | 1 (2.08) | ||
| Alcohol consumption, n (%) | No | 33 (67.35) | 36 (75.00) | (1)0.4056 (C) |
| Yes | 16 (32.65) | 12 (25.00) |
Clinical Parameters
Primary Outcomes
Table 3 presents the results of the analysis of change in K-WOMAC total scores measured at Baseline, 6 weeks, and 12 weeks in the primary analysis population, the PP Set. In the analysis of change in K-WOMAC total scores, at 6 weeks post-intake, the test group showed a decrease of 12.76 ± 15.13 points (p < 0.0001), while the control group showed a decrease of 9.08 ± 15.63 points (p = 0.0002). There was no statistically significant difference between the intake groups (p = 0.1508). At 12 weeks post-intake, the test group showed a decrease of 21.86 ± 15.98 points (p < 0.0001), whereas the control group showed a decrease of 14.92 ± 16.66 points (p < 0.0001). A statistically significant difference was observed between the intake groups (p = 0.0389).
Table 3. K-WOMAC: total score (PP set)| Test GroupN=49 | Control GroupN=48 | ||
| Visit 2 (Baseline) | Mean±SD | 37.69±17.00 | 37.02±16.61 |
| Min, Max | 8.00, 69.00 | 13.00, 69.00 | |
| p value (2) | 0.7949(W) | ||
| Visit 3 (6 weeks) | Mean±SD | 24.94±13.27 | 27.94±13.54 |
| Min, Max | 5.00, 59.00 | 4.00, 56.00 | |
| Change from baseline | Mean±SD | -12.76±15.13 | -9.08±15.63 |
| Min, Max | -49.00, 15.00 | -48.00, 20.00 | |
| p value (1) | <.0001 | 0.0002 | |
| p value (2) | 0.1508(W) | ||
| LS Mean±SE | -12.56±1.67 | -9.29±1.68 | |
| Diff LS Mean | -3.27 | ||
| 95% CI | -7.97, 1.44 | ||
| Visit 4 (12 weeks) | Mean±SD | 15.84±10.68 | 22.10±13.01 |
| Min, Max | 1.00, 60.00 | 0.00, 54.00 | |
| Change from baseline | Mean±SD | -21.86±15.98 | -14.92±16.66 |
| Min, Max | -56.00, 6.00 | -46.00, 20.00 | |
| p value (1) | <.0001 | <.0001 | |
| p value (2) | 0.0389(T) | ||
| LS Mean±SE | -21.62±1.57 | -15.16±1.59 | |
| Diff LS Mean | -6.45 | ||
| 95% CI | -10.88, -2.03 |
Table 4 presents the results of the analysis of change in K-WOMAC pain scores measured at Baseline, 6 weeks, and 12 weeks in the PP Set.
Table 4. K-WOMAC: pain score (PP set)| Test GroupN=49 | Control GroupN=48 | ||
| Visit 2 (Baseline) | Mean±SD | 7.37±3.66 | 6.85±3.41 |
| Min, Max | 2.00, 13.00 | 2.00, 13.00 | |
| p value (2) | 0.4928(W) | ||
| Visit 3 (6 weeks) | Mean±SD | 4.61±2.89 | 5.13±3.10 |
| Min, Max | 1.00, 12.00 | 0.00, 11.00 | |
| Change from baseline | Mean±SD | -2.76±3.72 | -1.73±3.80 |
| Min, Max | -11.00, 7.00 | -10.00, 7.00 | |
| p value (1) | <.0001 | 0.0028 | |
| p value (2) | 0.2172(W) | ||
| LS Mean±SE | -2.58±0.40 | -1.91±0.41 | |
| Diff LS Mean | -0.66 | ||
| 95% CI | -1.81, 0.48 | ||
| Visit 4 (12 weeks) | Mean±SD | 2.90±2.33 | 4.10±2.92 |
| Min, Max | 0.00, 12.00 | 0.00, 11.00 | |
| Change from baseline | Mean±SD | -4.47±3.65 | -2.75±3.82 |
| Min, Max | -12.00, 4.00 | -10.00, 4.00 | |
| p value (1) | <.0001 | <.0001 | |
| p value (2) | 0.0157(W) | ||
| LS Mean±SE | -4.27±0.36 | -2.95±0.37 | |
| Diff LS Mean | -1.32 | ||
| 95% CI | -2.34, -0.30 |
In the analysis of change in K-WOMAC pain scores, at 6 weeks post-intake, the test group showed a decrease of 2.76 ± 3.72 points (p < 0.0001), while the control group showed a decrease of 1.73 ± 3.80 points (p = 0.0028). There was no statistically significant difference between the intake groups (p = 0.2172).
At 12 weeks post-intake, the test group showed a decrease of 4.47 ± 3.65 points (p < 0.0001), whereas the control group showed a decrease of 2.75 ± 3.82 points (p < 0.0001). A statistically significant difference was observed between the intake groups (p = 0.0157).
Table 5 presents the results of the analysis of change in K-WOMAC physical function scores measured at Baseline, 6 weeks, and 12 weeks in the PP Set.
Table 5. K-WOMAC: physical function (PP set)| Test GroupN=49 | Control GroupN=48 | ||
| Visit 2 (Baseline) | Mean±SD | 27.00±12.52 | 26.75±12.22 |
| Min, Max | 6.00, 49.00 | 8.00, 50.00 | |
| p value (2) | 0.8398(W) | ||
| Visit 3 (6 weeks) | Mean±SD | 17.88±9.96 | 20.38±9.83 |
| Min, Max | 3.00, 45.00 | 3.00, 40.00 | |
| Change from baseline | Mean±SD | -9.12±10.85 | -6.38±11.19 |
| Min, Max | -35.00, 15.00 | -37.00, 13.00 | |
| p value (1) | <.0001 | 0.0003 | |
| p value (2) | 0.1311(W) | ||
| LS Mean±SE | -9.05±1.21 | -6.45±1.22 | |
| Diff LS Mean | -2.60 | ||
| 95% CI | -6.01, 0.80 | ||
| Visit 4 (12 weeks) | Mean±SD | 11.10±7.89 | 15.79±9.82 |
| Min, Max | 1.00, 42.00 | 0.00, 38.00 | |
| Change from baseline | Mean±SD | -15.90±11.71 | -10.96±12.20 |
| Min, Max | -39.00, 7.00 | -32.00, 13.00 | |
| p value (1) | <.0001 | <.0001 | |
| p value (2) | 0.0447(T) | ||
| LS Mean±SE | -15.81±1.17 | -11.05±1.18 | |
| Diff LS Mean | -4.76 | ||
| 95% CI | -8.06, -1.47 |
In the analysis of change in K-WOMAC physical function scores, the test group showed a decrease of 9.12 ± 10.85 points (p < 0.0001) at 6 weeks post-intake, while the control group showed a decrease of 6.38 ± 11.19 points (p = 0.0003). There was no statistically significant difference between the intake groups (p = 0.1311).
At 12 weeks post-intake, the test group showed a decrease of 15.90 ± 11.71 points (p < 0.0001), whereas the control group showed a decrease of 10.96 ± 12.20 points (p < 0.0001). A statistically significant difference was observed between the intake groups (p = 0.0447).
Secondary Outcomes
Table 6 presents the results of the analysis of change in VAS scores measured at baseline, 6 weeks, and 12 weeks in the PP Set. In the analysis of change in VAS scores, at 6 weeks post-intake, the test group showed a decrease of 8.45 ± 8.83 mm (p < 0.0001), while the control group showed a decrease of 5.85 ± 10.01 mm (p = 0.0002). There was no statistically significant difference between the intake groups (p = 0.1786).
Table 6. VAS (mm) (PP Set)| Test GroupN=49 | Control GroupN=48 | ||
| Visit 2 (Baseline) | Mean±SD | 45.41±11.13 | 46.44±12.03 |
| Min, Max | 32.00, 68.00 | 32.00, 75.00 | |
| p value (2) | 0.8032(W) | ||
| Visit 3 (6 weeks) | Mean±SD | 36.96±10.65 | 40.58±14.60 |
| Min, Max | 18.00, 60.00 | 14.00, 74.00 | |
| Change from baseline | Mean±SD | -8.45±8.83 | -5.85±10.01 |
| Min, Max | -34.00, 8.00 | -27.00, 23.00 | |
| p value (1) | <.0001 | 0.0002 | |
| p value (2) | 0.1786(T) | ||
| LS Mean±SE | -8.56±1.30 | -5.74±1.32 | |
| Diff LS Mean | -2.83 | ||
| 95% CI | -6.50, 0.85 | ||
| Visit 4 (12 weeks) | Mean±SD | 27.59±11.56 | 34.63±16.58 |
| Min, Max | 7.00, 62.00 | 5.00, 70.00 | |
| Change from baseline | Mean±SD | -17.82±13.80 | -11.81±13.99 |
| Min, Max | -53.00, 13.00 | -45.00, 26.00 | |
| p value (1) | <.0001 | <.0001 | |
| p value (2) | 0.0359(T) | ||
| LS Mean±SE | -18.05±1.84 | -11.57±1.86 | |
| Diff LS Mean | -6.48 | ||
| 95% CI | -11.68, -1.27 |
At 12 weeks post-intake, the test group showed a decrease of 17.82 ± 13.80 mm (p < 0.0001), whereas the control group showed a decrease of 11.81 ± 13.99 mm (p < 0.0001). A statistically significant difference was observed between the intake groups (p = 0.0359).
Safety Evaluation
A safety evaluation was conducted as the primary analysis using the Safety Set. A total of 60 participants from the test group and 60 participants from the control group who had consumed the investigational product at least once after randomization, were included in the analysis. Table 7
Table 7. Biochemical test| Test GroupN=60 | Control GroupN=60 | p-value2 | ||||
| n | Mean ± SD | N | Mean ± SD | |||
| AST (GOT)(IU/L) | Baseline (Visit 1) | 60 | 24.72±8.39 | 60 | 23.88±6.53 | 0.6358(W) |
| 12 weeks (Visit 4) | 58 | 23.98±6.14 | 59 | 23.80±6.84 | ||
| Change from baseline | 58 | -0.93±7.60 | 59 | -0.14±6.52 | 0.5242(W) | |
| p-value (1) | 0.3549 | 0.8737 | ||||
| ALT (GTP)(IU/L) | Baseline (Visit 1) | 60 | 18.70±13.52 | 60 | 18.08±9.90 | 0.8809(W) |
| 12 weeks (Visit 4) | 58 | 17.55±9.71 | 59 | 18.20±10.29 | ||
| Change from baseline | 58 | -1.16±11.12 | 59 | 0.10±9.00 | 0.2768(W) | |
| p-value (1) | 0.4322 | 0.9311 | ||||
| Total Cholesterol(mg/dL) | Baseline (Visit 1) | 60 | 194.60±38.79 | 60 | 194.18±45.50 | 0.9570(T) |
| 12 weeks (Visit 4) | 58 | 196.62±33.42 | 59 | 192.95±40.41 | ||
| Change from baseline | 58 | 1.62±24.78 | 59 | -1.64±26.25 | 0.5725(W) | |
| p-value (1) | 0.6203 | 0.6323 | ||||
| LDL Cholesterol(mg/dL) | Baseline (Visit 1) | 60 | 111.70±32.12 | 60 | 112.58±45.05 | 0.9018(T) |
| 12 weeks (Visit 4) | 58 | 113.28±30.12 | 59 | 109.27±35.83 | ||
| Change from baseline | 58 | 1.19±21.55 | 59 | -3.63±25.93 | 0.2128(W) | |
| p-value (1) | 0.6757 | 0.2871 | ||||
| HDL Cholesterol(mg/dL) | Baseline (Visit 1) | 60 | 62.70±15.68 | 60 | 61.52±13.78 | 0.6613(T) |
| 12 weeks (Visit 4) | 58 | 62.36±13.92 | 59 | 62.75±15.39 | ||
| Change from baseline | 58 | -0.57±8.53 | 59 | 1.46±8.17 | 0.2883(W) | |
| p-value (1) | 0.6135 | 0.1757 | ||||
| Triglyceride(mg/dL) | Baseline (Visit 1) | 60 | 113.67±53.54 | 60 | 114.68±110.15 | 0.0966(W) |
| 12 weeks (Visit 4) | 58 | 112.26±55.75 | 59 | 111.75±65.89 | ||
| Change from baseline | 58 | -0.79±42.55 | 59 | -4.00±80.44 | 0.1417(W) | |
| p-value (1) | 0.8876 | 0.7039 | ||||
| BUN(mg/dL) | Baseline (Visit 1) | 60 | 14.40±3.81 | 60 | 14.56±3.83 | 0.7988(W) |
| 12 weeks (Visit 4) | 58 | 14.41±4.98 | 59 | 14.58±4.16 | ||
| Change from baseline | 58 | -0.06±3.25 | 59 | 0.06±3.83 | 0.8578(T) | |
| p-value (1) | 0.888 | 0.9083 | ||||
| Creatinine(mg/dL) | Baseline (Visit 1) | 60 | 0.74±0.17 | 60 | 0.72±0.17 | 0.2900(W) |
| 12 weeks (Visit 4) | 58 | 0.75±0.21 | 59 | 0.73±0.19 | ||
| Change from baseline | 58 | 0.01±0.08 | 59 | 0.02±0.08 | 0.4467(W) | |
| p-value (1) | 0.4485 | 0.1291 | ||||
The evaluation included assessing the types and incidence rates of adverse events, as well as the severity of symptoms and their relationship with the investigational product. Additionally, analyses were performed on hematological and biochemical tests, vital signs (blood pressure, heart rate), and anthropometric measurements (body weight). Table 8
Table 8. Vital signs (blood pressure, pulse rate) and weight change| Test GroupN=60 | Control GroupN=60 | p-value2 | ||||
| N | Mean ± SD | N | Mean ± SD | |||
| Systolic blood pressure (mmHg) | Baseline (Visit 1) | 60 | 122.42±12.01 | 60 | 121.23±11.43 | 0.5814(T) |
| 12 weeks (Visit 4) | 58 | 121.71±11.70 | 59 | 122.36±9.80 | ||
| Change from baseline | 58 | -0.55±13.08 | 59 | 0.93±12.14 | 0.5259(T) | |
| p-value (1) | 0.7492 | 0.5575 | ||||
| Diastolic blood pressure (mmHg) | Baseline (Visit 1) | 60 | 76.60±9.25 | 60 | 76.08±8.19 | 0.7466(T) |
| 12 weeks (Visit 4) | 58 | 74.81±7.72 | 59 | 74.37±8.75 | ||
| Change from baseline | 58 | -1.74±8.42 | 59 | -1.63±9.54 | 0.9454(T) | |
| p-value (1) | 0.1206 | 0.1953 | ||||
| Pulse rate (회/min) | Baseline (Visit 1) | 60 | 76.45±9.11 | 60 | 74.68±11.02 | 0.1413(W) |
| 12 weeks (Visit 4) | 58 | 76.50±9.20 | 59 | 72.59±9.88 | ||
| Change from baseline | 58 | -0.03±9.85 | 59 | -1.78±9.87 | 0.3403(T) | |
| p-value (1) | 0.9788 | 0.1713 | ||||
| Weight (kg) | Baseline (Visit 1) | 60 | 61.86±12.24 | 60 | 63.35±12.04 | 0.4311(W) |
| 12 weeks (Visit 4) | 58 | 61.52±12.18 | 59 | 62.80±12.01 | ||
| Change from baseline | 58 | -0.14±1.09 | 59 | -0.33±1.05 | 0.3609(W) | |
| p-value (1) | 0.3373 | 0.0185 | ||||
There were no statistically significant differences observed between the consumption groups in any of the parameters measured in the biochemical tests after 12 weeks of consumption.
There were no statistically significant differences observed between the consumption groups in any of the parameters measured in the biochemical tests after 12 weeks of consumption.
Discussion
Joints are the regions where two or more bones come together. The ends of the bones that make up a joint are covered with cartilage, which provides a smooth surface, allowing for free movement without friction. When cartilage is damaged, abnormalities can occur in the bone underneath. Inflammation typically occurs in the process of cartilage destruction. With aging, cartilage can deteriorate, leading to deformities in the joints and localized degenerative changes. Osteoarthritis, which results from degenerative changes in joint cartilage, is primarily characterized by pain.1
The efficacy of na-hangwa extract powder has been confirmed in the MIA-induced osteoarthritis animal model, demonstrating its ability to alleviate pain. Moreover, in comparison to the MIA-induced group, the na-hangwa extract powder administration group showed significant reductions in inflammatory cytokines (IL-1β, IL-6, TNF-α), inflammatory mediators (LTB4, Osteocalcin, DPD, 5-LOX), COX-2, which induces inflammation and pain, as well as cartilage matrix-degrading enzymes (MMP-2, MMP-9). These findings validate the anti-inflammatory and cartilage-protective effects of na-hangwa extract powder. In this clinical trial, we aimed to investigate the efficacy and safety of DKB-131 (na-hangwa extract powder) on joint health in adult men and women with mild symptoms of knee osteoarthritis. Participants aged 40 to less than 80 years, with a baseline VAS score of 30 mm or higher (in the knee area) at Visit 1 and Visit 2, and with Kellgren & Lawrence Grade I or II on X-ray images of the knee joint were recruited for the study. Following 12 weeks of supplementation, we observed statistically significant improvements in the K-WOMAC total score, pain, physical function, and VAS functional level domain in the test group compared to the control group, indicating beneficial effects on joint health.
In the analysis of the change in K-WOMAC total score using the PP set, the test group showed a reduction of 21.86±15.98 points after 12 weeks of supplementation (p<0.0001), while the control group showed a reduction of 14.92±16.66 points (p<0.0001). A statistically significant difference was observed between the test and control groups (p=0.0389).
Regarding the change in K-WOMAC pain score analyzed using the PP set, the test group exhibited a reduction of 4.47±3.65 points after 12 weeks of supplementation (p<0.0001), whereas the control group showed a reduction of 2.75±3.82 points (p<0.0001). A statistically significant difference was observed between the intervention and control groups (p=0.0157).
Similarly, in the analysis of the change in K-WOMAC physical function score using the PP set, the test group demonstrated a reduction of 15.90±11.71 points after 12 weeks of supplementation (p<0.0001), while the control group exhibited a reduction of 10.96±12.20 points (p<0.0001). A statistically significant difference was observed between the intervention and control groups (p=0.0447).
In the analysis of VAS change using the PP set, the test group demonstrated a reduction of 17.82±13.80 mm after 12 weeks of supplementation (p<0.0001), while the control group exhibited a reduction of 11.81±13.99 mm (p<0.0001). A statistically significant difference was observed between the intervention and control groups (p=0.0359).
The WOMAC index exhibits high reliability in assessing the severity of knee and hip osteoarthritis, widely used as a tool for evaluating the severity of bone arthritis. Additionally, VAS is frequently employed as a self-assessment scale to evaluate the intensity of joint pain in clinical practice for patients with knee or hip osteoarthritis.13
During the course of the human clinical trial, a safety evaluation identified 3 cases in the test group and 6 cases in the control group with adverse events. However, both the study participants and investigators concluded that there was "no clear association" between the intake of the test food and these adverse events; thus, no serious adverse events occurred. Furthermore, there were no statistically significant differences observed in hematologic tests, biochemical tests, vital signs (pulse, blood pressure), or body weight after 12 weeks of intake.
In conclusion, based on the results of efficacy and safety evaluations, the intake of DKB-131 is deemed safe for human consumption and may contribute to joint health improvement.
Conclusions
Treatment options for osteoarthritis of the knee include surgery, lifestyle modifications, exercise, complementary and alternative therapies, and medication therapy. The Korean Orthopedic Association recommends weight loss and physical activity as part of the management of knee osteoarthritis. Drug therapies such as acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly used. However, acetaminophen carries a potential risk of liver damage, while NSAIDs pose risks of gastrointestinal complications such as ulcers and perforations.5
As evidenced by increasing concerns over the side effects and long-term burdens associated with the use of conventional medications, there has been a rise in the demand for dietary supplements targeting joint health in recent years. Reflecting this trend, products aimed at joint and bone health accounted for as much as 13% of the total production of individually recognized functional health foods in South Korea in 2010, indicating a substantial proportion of the market focus in this area.5.
In this context, DKB-131 has demonstrated efficacy in reducing pain and improving physical function compared to a placebo. Therefore, DKB-131 could serve as a promising alternative for the management of mild osteoarthritis, providing a favorable option for patients seeking relief from joint discomfort and improved mobility.
Funding
This research was supported by INNOPOLIS Foundation of Korea grant number 2022-D D-RD-0465. The funders had no role in designing the experiment or publishing the manuscript.
References
- 1. (2020) Bone and joint health related, Health functional foods (Evaluation Guide),Ministry of Food and Drug Safety,.09.
- 2.E Y Cheon. (2005) The Effects of a Self-Management Program on Physical Function and. , Quality of Life of Patients with Knee OsteoarthritisJournal of Korean Academy of Nursing 35(3), 514-525.
- 3.Jang M, Y M Lim. (2019) . Effects of Auricular Acupressure on Joint Pain, Range of Motion, and Sleep in the Elderly with Knee Osteoarthritis.Journal of Korean Academy of Community Health Nursing 30(1), 79-89.
- 4.S H Baek, S Y Kim. (2013) . , Pharmacologic treatment of osteoarthritis.Journal of the Korean Medical Association 56(12), 1123-1131.
- 5.D E Nam, O K Kim, T J Shim, J H Kim, Lee J. (2014) Effectof Boswellia serrata extracts on degenerative osteoarthritis in vitro and in vivo models.Journal of the Korean Society ofFood Scienceand Nutrition. 43(5), 631-640.
- 6.J S, J H Lee. (2012) Phytochemical and pharmacological aspects ofSiraitiagrosvenorii. Luo Han Kuo,Oriental Pharmacy and Experimental Medicine,12 233-239.
- 7.M J Kim, S H Yoo, Jung S, M K Park, J H Hong. (2015) Relative sweetness, sweetness quality, and temporal pro file of xylooligosaccharides and luo han guo (Siraitiagrosvenorii) extract,Food. , Science and Biotechnology 24, 965-973.
- 8.Kasai R, R L Nie, Nashi K, Ohtani K, Zhou J et al. (1989) Sweet cucurbitane glycosides from fruits ofSiraitiasiamensis(chi-zi luo-han-guo), a Chinese Folk Medicine,Agricultural Biological Chemistry53. 3347-3349.
- 9.Lu F, Li D, Fu C, Liu J, Huang Y et al. (2012) Studies on chemical fingerprints ofSiraitiagrosvenoriifruits (Luo Han Guo) by HPLC,Journal of Natural Medicine66. 70-76.
- 10.Kamei C, Sugiura M. (2005) New pharmacological functions of Luo Han Guo,Foods and Food Ingredients. , Journal of Japan,210 244-254.
- 11.Y M Lee, Kim M, H J Yuk, S H Kim, D S Kim.. (2023)SiraitiagrosvenoriiResidual Extract Inhibits Inflammation in RAW 264.7 Marcrophages and Attenuates Osteoarthritis Progression in a Rat Model,Nutrients,15 1-18.